If you’ve been dealing with chronic back pain, a herniated disc, or sciatica, there’s a good chance someone has mentioned spinal decompression therapy as a potential solution. And if you’re like most people, your very next question is: will my insurance actually pay for this?
It’s a fair question, and the answer isn’t as straightforward as you might hope. This guide breaks down everything you need to know about spinal decompression coverage, what insurers typically look for, and how to avoid unexpected out-of-pocket expenses before you book your first session.
What Is Spinal Decompression Therapy, Exactly?
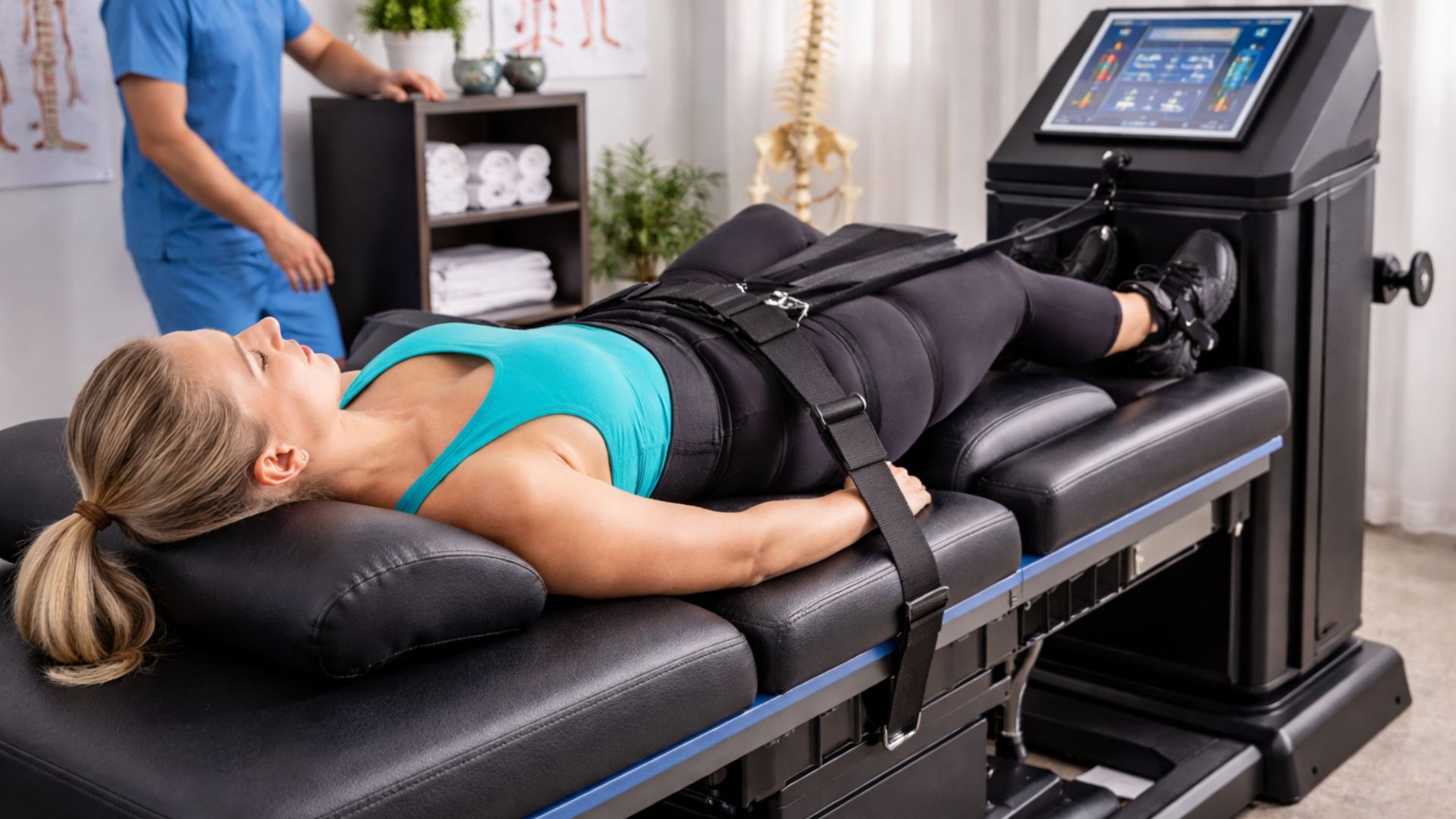
Before diving into the insurance side of things, it helps to understand what this therapy actually is. Spinal decompression therapy is a non-surgical treatment that gently stretches the spine using a motorized traction table. The goal is to relieve pressure on spinal discs and spinal nerves by creating negative pressure within the disc itself.
This therapy is a non-invasive treatment designed to relieve pain caused by bulging or herniated discs, degenerative disc disease, spinal stenosis, and related spinal conditions. If you’re curious about what spinal decompression therapy involves in more detail, it’s worth reading up before your consultation.
Decompression involves slow, controlled movements that encourage retraction of herniated disc material and improved circulation around the intervertebral disc. Many patients report significant pain relief after a series of sessions, often without the need for surgery, medication, or extended downtime.
Does Insurance Cover Spinal Decompression Therapy?
This is the big question, and the honest answer is: it depends. Whether spinal decompression is covered by insurance varies based on your plan, your provider, and how the treatment is documented by your clinic.
Most private insurance companies classify non-surgical spinal decompression therapy as an elective or experimental procedure.
That classification often means they won’t cover it, or they’ll only cover it under very specific conditions. However, coverage may still exist depending on how your provider codes the treatment and whether it’s bundled with other covered services.
What Insurance Companies Typically Look For
When evaluating a claim for spinal decompression therapy covered under your policy, insurers generally want to see the following:
- A confirmed medical diagnosis, often supported by MRI (magnetic resonance imaging) or X-ray imaging
- Documentation of medical necessity from a licensed provider
- Evidence that conservative treatments like chiropractic adjustments or physical therapy were attempted first
- A structured treatment plan with clear goals and responses to treatment milestones
Without these elements, even plans that technically allow coverage for spinal decompression therapy may still deny the claim.
Is Spinal Decompression Covered by Insurance Through Medicare?
Medicare is a common concern, especially for older adults dealing with chronic pain or degenerative disc disease. The short answer is that Medicare does not directly cover non-surgical spinal decompression therapy as a standalone procedure. Medicare may cover chiropractic adjustments, but decompression therapy as a standalone service is generally not reimbursed.
If you’re navigating Medicare and wondering about your options, it’s worth exploring whether Medicare covers chiropractic care in Walnut Creek to understand what is and isn’t included under your plan.
Medicaid coverage follows a similar pattern, but specific spinal decompression services are rarely listed as covered services under standard Medicaid plans. That said, every policy is different, so verification is always the right first step.
Spinal Decompression vs. Other Treatment Options
One reason insurance companies are slow to cover non-surgical spinal decompression is how it compares to other treatment options in terms of documentation and standardization. Physical therapy, chiropractic care, and even surgical interventions like spinal fusion or laminectomy have well-established Current Procedural Terminology (CPT) codes that insurers recognize.
Decompression therapy is a non-surgical treatment that is still gaining wider clinical recognition.
While the effectiveness of spinal decompression has been supported by a growing body of research, it is still gaining wider clinical recognition and is often coded differently across clinics, which creates inconsistency when insurers evaluate claims.
Chiropractic care, massage therapy, and physical therapy are more commonly reimbursed, and many patients choose to explore spinal decompression as a non-surgical alternative after those approaches provide only partial relief.
Navigating Insurance: Tips Before You Start Treatment
Navigating insurance before starting treatment can save you a lot of frustration. Here’s what to do before booking your first appointment:
Call your insurance provider directly. Ask specifically about coverage for spinal decompression therapy and request information about your deductible, co-pay, and any prior authorization requirements. Use the phrase “non-surgical spinal decompression” when asking, as this is how it’s typically categorized.
Request insurance verification from your clinic. A good clinic will assist with insurance verification before your first visit. This helps clarify what your plan covers, what requires pre-approval, and what your estimated out-of-pocket expense will be.
Ask about bundled billing. In some cases, coverage options improve when decompression is billed alongside chiropractic adjustments, physical therapy services, or pain management visits that are already covered.
Get the diagnosis in writing. Insurance reimbursement often hinges on how well the primary care physician or chiropractor documents the spinal conditions being treated – whether that’s disc herniation, sciatica, spinal stenosis, or low back pain.
For more detailed guidance, check out this resource on how to know if your chiropractic care is fully covered by insurance, and review the top insurance plans that cover chiropractic care in Walnut Creek to see which providers tend to be more accommodating.
The Average Cost of Spinal Decompression Therapy Without Insurance
If coverage for spinal decompression therapy isn’t available through your plan, it’s important to understand what you’re looking at out of pocket. The average cost of spinal decompression therapy per session typically ranges from $30 to $200, depending on the clinic and the length of the session. A full treatment plan often includes 15 to 30 sessions, meaning total costs can range from a few hundred to several thousand dollars.
Many clinics offer payment plans or package pricing to make therapy more accessible. Spinal decompression therapy can significantly support long-term spinal health, and for many patients, the cost feels worthwhile compared to surgery or ongoing chronic pain management over time.
Frequently Asked Questions About Spinal Decompression
Is decompression therapy a non-invasive option for everyone with back pain?
Spinal decompression therapy is generally safe for many patients with disc-related back pain, but it’s not appropriate for everyone. Conditions like fractures, tumors, or certain types of spinal fusion hardware may make someone a poor candidate. A proper evaluation at a qualified clinic will determine if this treatment is the right fit.
Can therapy be combined with other chiropractic care?
Yes. Decompression therapy is generally performed alongside chiropractic adjustments, exercise, and other supportive treatments. A personalized treatment plan often delivers better results than decompression alone.
Is spinal decompression the right choice for herniated discs?
Spinal decompression therapy offers a non-surgical path for patients dealing with herniated disc pain, disc bulge, facet syndrome, and related spinal conditions. Many patients find it effective when other approaches haven’t provided lasting relief. For those looking into spinal decompression therapy for chronic back pain, it’s worth speaking with a qualified spinal decompression chiropractor to see if decompression is the right fit for your specific spinal condition.
Conclusion
Insurance coverage for spinal decompression therapy is inconsistent, but that doesn’t mean the therapy itself isn’t worth exploring. Understanding your policy, getting the right documentation, and working with a clinic that handles insurance verification can make a real difference.
At Elite Chiropractic Rehab and Wellness in Walnut Creek, the team is committed to helping you understand your coverage options and build a plan that works. Call 925-476-5070 or visit our website to take the first step toward a pain-free future.